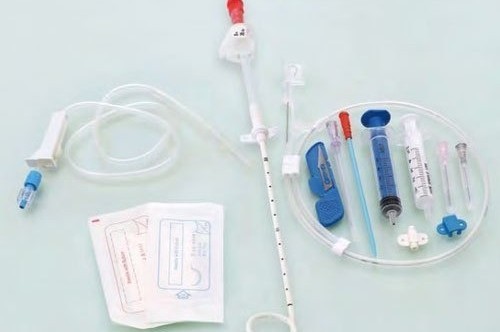
Engineering Chest Drainage Catheters for Safety and Ease of Use in Thoracic Care
In thoracic care, precision and reliability are not optional, they are critical. Whether managing pneumothorax, pleural effusion, hemothorax, or post-operative fluid accumulation, chest drainage procedures require devices that perform consistently under sensitive and high-risk conditions. At the center of these interventions lies a vital tool: the chest drainage catheter.
Modern advancements in chest drainage catheter design have significantly improved both patient safety and clinical efficiency. Engineering today goes beyond simple fluid evacuation, it integrates material science, ergonomic considerations, and safety mechanisms to support better outcomes in thoracic care.
The Critical Role of Chest Drainage in Clinical Practice
Chest drainage is commonly performed in emergency medicine, trauma care, thoracic surgery, and intensive care units. The objective is straightforward: remove air, blood, or fluid from the pleural space to restore normal lung expansion. However, the procedure itself involves potential risks, including tissue trauma, infection, improper placement, and drainage inefficiency.
Complications such as catheter kinking, blockage, or dislodgement can delay recovery and increase hospital stay duration. Therefore, device design directly influences procedural success, patient comfort, and overall safety.
Material Science: Strength Without Rigidity
One of the most important aspects of chest drainage catheter engineering is material selection. The catheter must be strong enough to maintain structural integrity, yet flexible enough to conform to anatomical contours.
Modern chest drainage catheters are typically made from biocompatible, medical-grade polymers that balance durability with flexibility. These materials reduce irritation of surrounding tissues while preventing collapse under negative pressure conditions. Flexibility is particularly important during patient movement, as rigid catheters increase discomfort and the risk of tissue damage. Kink-resistant design ensures uninterrupted drainage, which is essential for maintaining lung re-expansion and preventing fluid accumulation.
Atraumatic Design for Safer Insertion
Insertion is a critical phase of chest drainage procedures. Traditional rigid tubes often required more force during placement, increasing tissue trauma and patient discomfort. Today’s engineered catheters incorporate:
- Smooth, atraumatic tips to reduce tissue injury
- Controlled stiffness gradients that assist with guided placement
- Precision side ports to enhance drainage efficiency
Atraumatic tip design minimizes damage to surrounding structures while improving clinician control during insertion. This is especially vital in emergency settings where rapid but precise action is required.
Optimized Drainage Performance
Effective drainage depends on more than insertion, it requires consistent lumen integrity and fluid flow. Modern chest drainage catheters are designed with:
- Smooth internal lumens to prevent clot adhesion
- Multiple strategically positioned drainage eyes for uniform evacuation
-
Radiopaque markers to confirm accurate placement under imaging
Flow efficiency plays a significant role in preventing complications such as retained hemothorax or incomplete fluid evacuation. A well-designed catheter supports continuous drainage without frequent repositioning or replacement. Manufacturers such as MedivationBio focus on engineering catheters that combine structural strength with optimized flow pathways, helping clinicians maintain predictable drainage performance across varied thoracic conditions.
Ease of Handling for Clinical Teams
In thoracic care, device usability is as important as performance. Chest drainage procedures often occur in high-pressure environments such as trauma bays or intensive care units. Devices must therefore be intuitive, ergonomic, and reliable. Features that enhance ease of use include:
- Clear depth markings for accurate insertion guidance
- Secure connectors that prevent accidental disconnection
- Flexible tubing compatibility with drainage systems
By simplifying handling and reducing procedural complexity, well-engineered catheters support clinician confidence and efficiency.
Infection Prevention and Sterility
Like all invasive devices, chest drainage catheters must maintain the highest sterility standards. Healthcare-associated infections can significantly impact patient recovery and outcomes. Modern manufacturing processes incorporate:
- Controlled cleanroom production environments
- Validated sterilization techniques
- Protective packaging that preserves sterility until point of use
Sterility assurance, combined with biocompatible materials, reduces the risk of catheter-related infections and supports safer thoracic interventions.
Addressing Diverse Clinical Scenarios
Chest drainage requirements vary depending on patient condition. Trauma patients may require rapid, large-volume evacuation, while post-surgical patients may need controlled, long-term drainage. Engineering versatility into catheter design allows for:
- Multiple size options to match clinical needs
- Variable stiffness for different insertion techniques
- Compatibility with both emergency and elective thoracic procedures
This adaptability ensures that devices can meet the demands of diverse healthcare environments.
The Future of Thoracic Drainage Device Engineering
As healthcare continues to prioritize patient-centered care and measurable outcomes, chest drainage catheter design will evolve further. Innovations in material science, surface coatings, and ergonomic enhancements will continue to reduce complications and improve comfort.
Ultimately, chest drainage catheters may appear simple, but their engineering reflects a complex integration of safety, strength, and usability. By aligning device design with clinical realities, modern thoracic care can achieve safer procedures, faster recovery, and improved patient confidence. In high-risk thoracic interventions, thoughtful engineering is not just about function, it is about trust, precision, and better outcomes at every step of care.
